*We acknowledge our use of the “click-bait” title but if you’re reading this, it worked! Hopefully you enjoy the jest if you read to the end. We always welcome your feedback on titles and blog post ideas, so please email us at social@bodygears.com
Whether you’re struggling to put luggage in an overhead compartment or you’d just like to be able to reach into the back seat of the car without pain, you’ve come to the right place. People can be quick to resort to surgery when shoulder pain comes out of nowhere and doesn’t resolve in a reasonable amount of time. It’s easy for scary terms like “tears” and “bone spurs” to leave you thinking surgery must be you’re only option.
If you’re looking for a safe, effective and non-invasive treatment option that is designed to relieve pain resulting from a wide range of musculoskeletal conditions, sports injuries, workplace injuries and more, then physical therapy is for you. Shoulder pain can be caused by a number of different factors and physical therapists are experts at differentiating symptoms from true dysfunctions to narrow down the root cause of the problem. Below are 5 secrets about shoulder pain that can help you avoid surgery, just like many of our patients.
1. Tendinitis/Tendinopathy/Tendinosis Are Symptoms of a Bigger Problem
Finding the root cause of an injury in the medical field can result in variable answers because it depends on how far back in the timeline you and the clinician want to go. Initially, identifying the injured structure (such as whether it’s a biceps or supraspinatus tendon injury) is important but it’s a big mistake to stop there and simply direct all treatment (medications, modalities, exercises) at the tendon.
The natural next question is, how did this happen? “Repetitive strain”, “wear and tear”, and “overuse” are often proffered here and this is usually where the search for the root cause will end. The problem with this is that people tend to do one of three things (or all of them) with this kind of answer: 1. Decide to stop doing the things they love (like tennis) and the things they need to do (like wash their backs); 2. Assume they need surgery to replace or repair their withering parts; 3. Accept their fate as someone who will always have a bad shoulder, will feel worse with bad weather, rely on medications, and invent some sort of shoulder circle stretch that never makes them feel better but conveys to others the level of discomfort they’re in.
People who get better take the search for the root cause just one step further with the help of their physical therapist and identify whether they have an ergonomics issue and/or a mechanics issue.
If your tendon pain resulted from activities you’re unable to avoid, such as tasks that are part of your job description or household chores, then taking a look at the ergonomics (how to alter the task to fit your body), will provide a long-term solution for reducing the stress on the tendon. For activities that slowly became more painful over time, you likely have a mechanics issue that is placing unnecessary stress on your tendon instead of spreading the load efficiently across the rest of the tissues. Physical therapists are experts in human movement and will be able to identify which aspect of your shoulder mechanics to change to offload your painful tendon, allowing it to heal and prevent future or further injury.
2. Rotator Cuff Tears Are Symptoms of a Bigger Problem
First, let’s distinguish that a “tear” indicates part of the muscle is damaged while a “rupture” indicates the entire muscle belly has been severed. Surgery is indicated typically for traumatic rotator cuff ruptures where the two ends have moved too far away for natural healing to occur between them.
Did you know, it’s possible to have a rotator cuff rupture and not even know about it? 23% of people are walking around with full ruptures they’re not even aware of (asymptomatic) and that number jumps to 51% after 801. The two big takeaways from those shocking numbers are: 1. It’s the quality of your function rather than the state of your tissues that dictates the need for intervention, and 2. If this is something you’ve potentially been walking around with for a while before it became symptomatic, then it’s not something you need to rush to surgery for.
So, what’s the bigger problem these tears stem from? A mechanics issue involving poor control of the shoulder blade (which includes the shoulder socket – it’s not just the arm bone that moves in the socket, the orientation of the socket needs to change too). For the official explanation, we’ll quote the research so you can be sure we haven’t made this up.
“In patients exhibiting rotator cuff tears and/or subacromial impingement, altered muscular activity or strength, and changes in the timing properties of the serratus anterior the upper, middle and lower portions of the trapezius are frequently observed. Specifically, it has been consistently shown that decreased serratus anterior strength, hyperactivity and early activation of upper trapezius, and decreased activity and late activation of middle and lower trapezius are present in patients with shoulder pain and pathology.”1
If you got one thing out of that paragraph, hopefully it’s a sense of motivation to start strengthening your serratus anterior muscles. And make an appointment with your physical therapist (TIP: everything listed in that paragraph is fixable with physical therapy).
1. Edwards, Peter, et al. “Exercise rehabilitation in the non-operative management of rotator cuff tears: a review of the literature.” International journal of sports physical therapy 11.2 (2016): 279.
3. Shoulder Bursitis Is a Symptom of a Bigger Problem
The subacromial bursa is a small sack of fluid that acts as a friction-reducing divider between the supraspinatus and deltoid tendons so they can glide easily next to each other. As you can see in the image below, there’s not a lot of space between the shoulder capsule and the acromion (part of the shoulder blade), so if the bursa grows a little due to inflammation, it’s going to make shoulder movements a lot more difficult and painful.
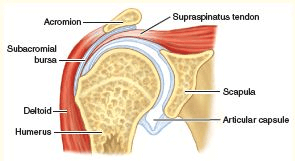
We can be quick to blame the bursa and stick it with needles full of corticosteroids as punishment for taking up so much space, but your poor bursa is the victim in all this! There are two common mechanics issues that are behind bursitis and you may even have a little of both.
The first is a shoulder blade movement dysfunction where the acromion (see picture – it’s a protrusion of the shoulder blade) isn’t getting out of the way during shoulder motions. As referred to briefly in the section above, the shoulder blade should rotate upwards, move to the side, and tilt backwards when you raise your arm. If it isn’t doing those things (possibly because the right muscles aren’t turning on or aren’t strong enough), the acromion can compress your bursa.
The second mechanics issue is a humerus/arm bone dysfunction where the bone rides too high in the joint. Ask one of our physical therapists about the convex on concave rule and they’ll be all too pleased to explain this mechanics issue to you with our skeleton, George.
4. Labral Tears Are a Symptom of a Bigger Problem
Labral tears due to acute injuries, like a fall on an outstretched hand or bracing yourself in a car accident, are not uncommon and are obviously not a symptom of a motor dysfunction. However, tears sustained by overhead athletes (like baseball players and weight lifters) or tears that happen to show up on your MRI are indicative of an area of increased stress in your shoulder.
Again, the instinct is to go in and sew up that labral tear, but when the anesthesia wears off, you’re just going to keep moving the way you always have and keep stressing out that same part of your labrum (meaning the pain doesn’t go away).
In some cases with severe tears, surgery is necessary to restore structural integrity and not have a flap of labrum disrupting other tissues, but guess where your next stop after surgery is? To see your friendly physical therapist to restore efficient shoulder motion.
For those who don’t experience severe instability with their labral tears, physical therapy will restore efficient shoulder motion (emphasis on the will because if you don’t see results with one physical therapist, don’t write off the rest of us! The worst and best thing about physical therapy is that each therapist has a different approach. Keep searching until you find someone who works for you).
5. Shoulder Bone Spurs Are a Symptom of a Bigger Problem
Despite having a name that conjures images of sharp spikes protruding from a cowboy’s heel, bone spurs are usually smooth areas where a little extra bone has been laid down. It’s just that “bone mounds” isn’t as fun to say.
Just like labral tears, bone spurs occur when one area of the shoulder is being singled out to take the forces that should be evenly spread throughout the whole shoulder complex. Your body is actually trying to help you by reinforcing that area with more bone to prevent a stress fracture but the trade-off is that extra bone takes up a little space in an already narrow opening. You can help your body (and get rid of your pain) by changing your mechanics to stop stressing out that bony area.
Physical Therapy Can Provide Fast Relief for Shoulder Pain
Hopefully, you’ve picked up on the theme of this blog post, but to tie it all up nicely: your shoulder pain is likely a symptom of inefficient mechanics, ergonomics, or both. How you move has the biggest impact on the health of your tissues, with the ability to both nurture and degrade them.
If you or a loved one have been experiencing recurrent or prolonged shoulder pain, speak with one of our physical therapists as soon as possible. Physical therapy is a safe, non-invasive and holistic treatment option that can help people of all ages and activity levels. Call one of our 6 Illinois offices today to learn more about the benefits of physical therapy and begin your journey toward living a pain-free life!
Written by: Dr. Julia Melanson, PT, DPT
Edited by: April Oury, PT, MSPT, IOC, CFMT, FAAOMPT, Founder
As always, consult with your Licensed Physical Therapist for individualized advice. For those in Illinois, visit your PT immediately without a prescription or referral.
Give us a call at (877) 709-1090 for more information or fill out the contact us form and we will contact you.
Don’t forget to check out our Instagram, Facebook, and Podcasts for more great information and resources.
Copyright © 2019 by Body Gears Physical Therapy
All rights reserved. This blog or any portion thereof may not be reproduced or used in any manner whatsoever without the express written permission of the publisher except for the use of brief quotations in a review.






